
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
© Marzena Seledyn, 2025
© Alicja Moczydłowska, 2025
© Ewa Perkowska, 2025
© Zoia Sharlovych, 2025
Український педагогічний журнал ⚬ 2025 ⚬ № 1
Marzena Seledyn, Master of Nursing, ward nurse of the Medical Care Association in Szczytno, supervisor of clinical practice students, International Academy of Applied Sciences in Łomża, Łomża, Republic of Poland
https://orcid.org/0009-0004-7524-9166
Alicja Moczydłowska, PhD in Health Sciences, Deputy Dean for Organizational Affairs, Head of the Department of General Patient Care, Adjunct Professor, International Academy of Applied Sciences in Łomża, Łomża, Republic of Poland
https://orcid.org/0009-0006-5255-8809
amoczydlowska.wsa@wp.plam805@lomza.mans.edu.pl
Ewa Perkowska, Adjunct Professor, Faculty of Health Sciences, Medical University of Białystok, Republic of Poland
https://orcid.org/0000-0002-0815-216X
Zoia Sharlovych, Candidate of Pedagogical Sciences, Vice-Dean for International Affairs, Adjunct Professor, International Academy of Applied Sciences in Łomża, Łomża, Republic of Poland
https://orcid.org/0000-0001-8115-9838
Aggression in the modern world is evolving and becoming increasingly prevalent. The phenomenon of patients' aggression towards medical staff in the work environment is becoming more and more frequent.
The aim of the study is to diagnose the phenomenon of patient aggression towards medical staff, including nursing teams.
The research was conducted using a diagnostic survey method in the organizational units of Szpital Powiatowy in Szczytno. The research was carried out between March 15, 2022, and November 30, 2022, using a proprietary questionnaire.
The study involved 150 people, most of whom were women. The study showed that 97% of respondents experienced aggression from patients, including 66% verbal aggression and 34% physical aggression. The study results also showed a correlation between patients' aggression and its impact on the behavior of healthcare workers, causing nervousness in 50% of them. The respondents declared a negative impact of aggression on their work, disorganizing it (30%) and on bio-psycho-social well-being, causing nervousness (26%), and discouragement from work (18%).
Physical and verbal aggression from patients is still a very common phenomenon in health care. Medical staff often experience psychological aggression from patients and/or their relatives. According to the respondents, new forms of aggression, such as hate speech or stalking, were experienced, caused by patients and their families towards medical staff, but they occurred quite sporadically. Patients' aggression towards medical staff always leaves negative health effects, mainly in the emotional sphere of medical staff. The staff expects training in the field of employee rights protection and ways of dealing with aggressive patients.
Keywords: aggression, patient, medical staff, hate, stalking
Aggression in the modern world is evolving and becoming an increasingly common phenomenon. In recent years, there has been a dynamic increase in the phenomenon of aggression together with the violence, cruelty and ruthlessness associated with it, and in some cases even organizational perfectionism. The present world is full of information about the popularity of aggression, where people become its victims. Therefore, aggression in our consciousness changes our emotional landscape, appears as an element of everyday life not only in the social but also professional context, and also becomes a fragment of the information system, entertainment and mass culture.1
The World Health Organization (WHO) does not define aggression, but it does define violence in the workplace as incidents in which workers are overexploited, threatened or attacked in circumstances related to their work, including commuting to and from work, involving an explicit or implicit challenge to their safety, well-being or health.2
Aggression towards healthcare workers usually results from rather excessive and unrealistic expectations, demands and requests from patients and often from their families, but also from instrumental and objective treatment of the staff. All employees are exposed to patient aggression, but nurses and medical carers are at high risk due to their direct care of patients. Hospitalisation disrupts their daily rhythm, plans and commitments and it is associated with a loss of security, independence, fear for health and life. A hospital stay may often cause very strong stress, which initiates negative behaviours: aggression, hypochondria, alienation and demandingness.3
According to Drabek et al., their study showed that out of 1163 people taking part in the study, 56.75% of nurses experienced verbal aggression and 30.35% were subjected to physical aggression from patients.4
A very important issue worth paying attention to was the impact of patient aggression on the bio-psycho-social well-being of staff. The most, every fourth respondent, claimed that it causes nervousness. The next one is discouragement from work or a change in attitude towards work (18.0%). Other respondents reported sleep disorders, but also conflicts in the team. Bogucka M. shows similar data in her research. According to her results, about 30% of respondents also report nervousness, but 35.62% report discouragement from work. This is a very high percentage out of 100% of respondents.5
Anger in patients is most often caused by insufficient satisfaction of their expectations by the health care facility staff or by the desire to emphasize their supremacy. If the patient believes that by showing anger he/she stands in the way of overcoming an obstacle or so-called breaking the employee, he/she will activate his/her actions. Therefore, it mobilizes the energy that is needed in his/her opinion to reduce our inaction or helplessness.6
Aggressive behavior of patients may manifest itself through verbal arousal, i.e. verbal aggression, and physical arousal, i.e. violence in behavior. Due to the orientation of actions, aggressive behavior may take the form of autoaggression and actions directed against other patients or medical personnel. It has been found that many environmental and somatic factors may increase the risk of aggression.
Another factor contributing to the occurrence of aggressive behavior in patients is the improper and reprehensible conduct of medical staff. Most often, it is a lack of experience and commitment to work, a lack of empathy, insufficient feedback or even its complete absence, errors in communication as well as treating the patient as an object, cynicism of the staff and taking on the role of a judge, which provoke patients and their families to raise doubts and an outburst of aggressive behavior.7
The Supreme Medical Chamber and the Supreme Chamber of Nurses and Midwives, in order to protect their own professional groups and to enable doctors and nurses to report cases of aggression in the workplace, have created the "Monitoring Aggression in Healthcare" (MAWOZ) system. All over the world, healthcare workers are very often exposed to hate and aggression in their workplaces. Therefore, a thorough understanding of the problem, circumstances and places where they are particularly vulnerable allows for preventive actions to be taken.8
A procedure has been developed concerning the rules of conduct of a nurse or a midwife in the event of aggressive behaviour of a person during and in connection with the performance of activities consisting in the provision of health services referred to in Art. 4 sec. 1 points 1-5 and Art. 5 section 1 points 1-9 of the Act of July 15, 2011 on the professions of a nurse and a midwife (Journal of Laws No. 174, item 1039, as amended) benefiting from the protection provided for public officials in accordance with Art. 11 sec. 2 of the aforementioned Act.9,10,11,12
Many researchers of this problem report a huge amount of research and results confirming that patient aggression in its various forms leaves a mark on the psyche of medical professionals and has a huge impact on their professional work. Most of these studies were conducted using a diagnostic survey, the tool of which was a questionnaire. Increasingly often, scientific articles are written on their basis and procedures are introduced in health care institutions to facilitate the staff’s work with aggressive patients.13,14
Lickiewicz J. et al., presenting the research results in their work, state that shouting and threats are the most common symptoms of verbal aggression and constitute as much as 59.89% of all responses.15
Aggression is intentional actions that lead to psychological and physical harm. These are actions directed at the outside world or towards oneself, which are intended to cause harm. Aggression is also defined as actions undertaken by a person in an intentional manner, which are a threat or cause losses in the physical, psychological and social well-being of other people, i.e. they cause pain, suffering, lead to destruction and loss of appreciated values. 16
The phenomenon of aggression is a very complex problem, there are many theories on this topic, which have come from the pen of famous scientists and philosophers. The Covid-19 pandemic has brought an avalanche of aggressive behavior among patients. The Supreme Medical Chamber and the Supreme Chamber of Nurses and Midwives keep a register of monitoring aggression in health care institutions, and the statistics record the most dangerous cases. However, the number of aggressive behaviors of patients towards medical staff is much higher – it could be counted in thousands, but most cases are not recorded in the register. 17
It should be emphasized that there are no records in the Labor Code protecting employees against aggression. There is only a legal basis protecting against mobbing /Article 94(3) of the Labor Code/, which can also cause negative effects in terms of the bio-psycho-social state of the employee. 18
People who have been previously diagnosed with mental disorders manifesting themselves in attacks of aggression should remain under the supervision of doctors with a psychiatric specialty throughout the pandemic period and after its end, while people who have only developed this type of behaviour during the pandemic should seek advice from psychologists and should be treated pharmacologically with antidepressants. 19
Medical workers are most often exposed to attacks of aggression due to the nature of their work. An inherent element of their work is maintaining direct contact with a patient who suffers, requires help and often shows his/ her dissatisfaction and frustration leading to aggression. Long-term exposure to attacks of aggression from patients leads to negative emotional experiences: feeling fear, anger and a sense of helplessness. On the other hand, systematically repeated negative emotions lead to a situation in which the victim – the medical worker – transforms into the aggressor. 20
A slightly different position and behavior is presented in the scientific materials of Bilgin H., Tulek Z., Ozcan N. According to their research, 42.58% of the people surveyed suppress their anger, while about 40% say that they try to defend themselves and at the same time overpower the patient. 21
Assessment of the phenomenon of patient aggression towards medical staff, including nursing personnel:
1. Whether and how often medical staff, including nursing personnel is exposed to physical aggression from patients?
2. Whether and how often verbal, psychological/emotional violence/aggression from the patient or his/her family occurs?
3. Have any new forms of aggression like hate or stalking been recorded?
4. What is the impact of patient aggression on the bio-psycho-social well-being of medical staff?
5. Does medical staff require training on how to deal with aggressive patients?
6. What does legal protection of staff look like regarding the phenomenon of aggression?
Research hypotheses:
1. Physical aggression of patients towards staff is a common phenomenon in healthcare entities.
2. Verbal aggression on the part of the patient occurs with varying frequency and medical staff is exposed to it regardless of education level and position held.
3. Medical staff often experience psychological aggression from patients and/or their relatives.
4. New aggression phenomena (stalking, hate) occur sporadically.
5. Patient aggression towards medical staff always leaves negative health effects, mainly in the emotional sphere of the personnel.
6. Employees are familiar with legal protection in the fight against patient aggression, but require refresher training in dealing with aggressive patients in accordance with the law.
The concept of the conducted scientific research is the interpretation of events occurring in reality, which will make it easier to visualize them and predict when they occur. The obtained results of the undertaken research will be a factor in shaping conventions, imperatives and all guidelines beneficial to solving problems.22
The work uses the diagnostic survey method, which allows the researcher to learn about measurable social phenomena and determine their potential development and scope. The collected information will allow for the interpretation of the causes and consequences of the events that occurred, and will also help in planning the right solutions to the problem.
The research tool used was an original survey questionnaire that allowed for obtaining information on the problem of patient aggression towards medical staff and its impact on their bio-psycho-social well-being. The randomized study involved 150 medicians working in the Emergency Department and Primary Health Care of the District Hospital in Szczytno.
The study involved 150 people, the vast majority were women (81.0%), the largest research group were medicians over the age of 51 (42.0%), living in the city (71.0%) with their families (86.0%). The majority of the respondents were employees with secondary education (45.0%), every third respondent declared higher education (31.0%), and almost every fourth had a bachelor's degree. Detailed data are presented in Figure 1.
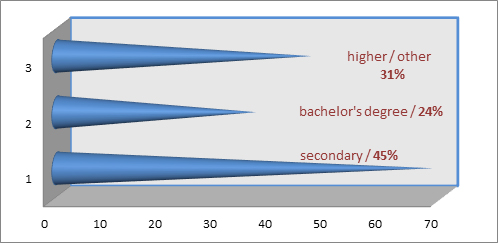
Figure 1. Education of the respondents.
Source: Own study.
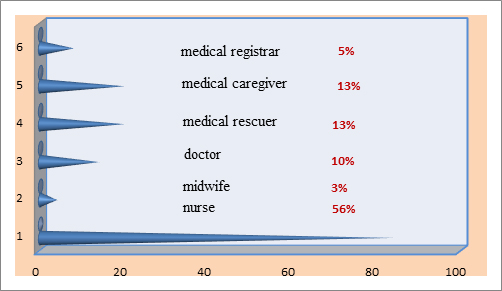
Figure 2. Occupation of the respondents.
Source: Own study.
The study involved employees from several medical professional groups, with the largest group being nursing staff (56.0%). The data is presented in Figure 2. The longest declared employment period is 30 years and over 30 years, which was indicated by almost every third respondent.
According to the surveyed employees, the largest group was made up of staff working in the internal department (31.0%) and in the Temporary Covid Department (17.0%). The data are presented in Table I.
Table I.
| No. | Department | percent |
|---|---|---|
| 1. | Internal Department | 31,0% |
| 2. | Surgical Department | 12,0% |
| 3. | Gynaecology and Obstetrics Department | 3,0% |
| 4. | Emergency Room / ER | 14,0% |
| 5. | Specialized hospital clinics | 4,0% |
| 6. | Night and Holiday Health Care | 2,0% |
| 7. | Emergency Aid Department | 7,0% |
| 8. | Temporary Covid Department | 17,0% |
| 9. | Social Welfare Home | 2,0% |
| 10. | Primary Health Care | 5,0% |
| 11. | Long-Term Home Care Nursing | 1,0% |
| 12. | Others/ CT laboratory, Analytical Laboratory | 2,0% |
| Sum | 100% |
Source: Own study.
According to the results of the study, problems related to patient aggression are still visible, as 97.0% of the respondents declared that they had encountered aggressive behavior on the part of patients in their professional work, while every third of them claimed that it was physical aggression and the rest indicated verbal aggression (66.0%). Quite often, both forms of indicated aggression occurred simultaneously. In terms of the frequency of patient aggression towards staff, the respondents were convinced that the event occurred in their work "quite often" (29.0%) or "sometimes" (45.0%).
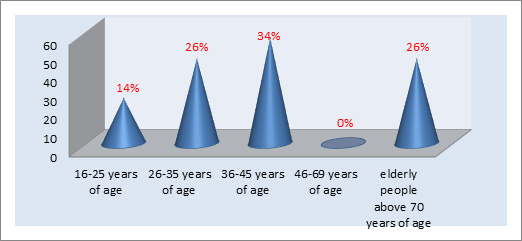
Figure 3.
Age groups of aggressive patients.
Source: Own study.
The most common aggressors, according to the respondents, were patients aged 36-45 (34.0%). The data are presented in Figure 3. The results of the study indicate that the gender of the patient with aggression was of no great importance (59%). In terms of the causes of patient aggression, the respondents indicated alcohol intoxication (23%), and the smallest percentage of aggressors were patients dissatisfied with the services provided to them. Detailed data are presented in Table II.
Tabel II.
| No. | Factors causing aggression | % |
|---|---|---|
| 1. | waiting time too long | 10% |
| 2. | dissatisfaction with the services provided | 8% |
| 3. | emotional aggression resulting from character traits | 17% |
| 4. | alcohol intoxication | 23% |
| 5. | intoxication with psychoactive substances | 13% |
| 6. | disease entity / mental illness | 15% |
| 7. | senile dementia | 14% |
| Sum: | 100% |
Source: Own study.
According to research, aggression among patients was most often manifested by using uncensored words, shouting or threats, and scaring the staff with the employer. Physical violence was indicated by 15.0% of the respondents. Data are presented in Table III.
Tabel III.
| No. | Aggressive behavior of patients | % |
|---|---|---|
| 1. | shout | 21% |
| 2. | threats, scaring | 20% |
| 3. | vulgarisms, name-calling, insults | 30% |
| 4. | threats using dangerous objects (knife, others) | 6% |
| 5. | physical violence, e.g. pushing, poking, spitting, biting, scratching | 15% |
| 6. | verbal and physical sexual harassment, including unwanted touching | 1% |
| 7. | destruction of public property | 8% |
| Sum: | 100% |
Source: Own study.
According to the respondents, the methods and preventive measures used most often in healthcare facilities were, for example: direct coercion (18.0%). Studies indicate that talking and trying to explain were the most effective forms of calming the patient down (39.0%). The data are presented in Figure 4.
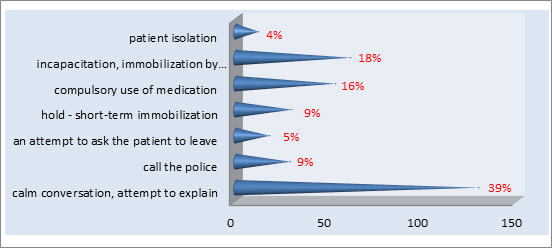
Figure 4. Preventive measures.
Source: Own study.
The majority of the surveyed claimed that patient aggression has a negative impact on the behavior and emotions of medical staff (65.0%), which may negatively affect the quality of their work. According to the surveyed, they may cause nervousness (50.0%), every fifth surveyed person indicated emotional distress and fear, anxiety and fear, anger and aggression and withdrawal. More than 3/4 of the surveyed believed that patient aggression has an impact on the work of medical staff (86.%), causing danger at work, including an increased risk of making a mistake, or causing burnout over some time. The reactions of the staff to verbal aggression are illustrated in Figure 5.
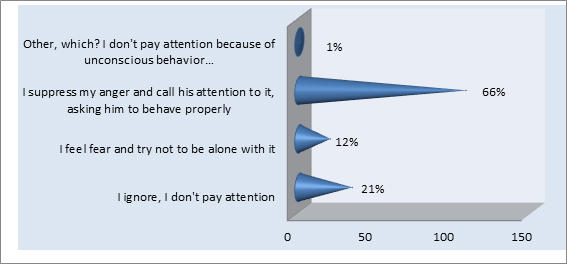
Figure 5. Staff reaction to verbal aggression.
Source: Own study.
Half of the respondents (50%) encountered psychological/emotional aggression from patients on average 1-2 times a month, which evoked many emotions, including anger (66.0%) (Figure 5). On the other hand, physical aggression forced medical personnel to behave in an unusual way, e.g. calling the police (34.0%) or defending themselves (36.0%). The data are presented in Table IV.
Tabel IV.
| Staff reaction | Percent |
|---|---|
| I retreat, I run away | 21% |
| I defend myself and try to overpower the patient. | 36% |
| I call for help (Police) | 34% |
| Other: tries to calm the patient down and call a doctor | 9% |
| Sum | 100% |
Source: Own study.
Almost every third respondent indicated experiencing new forms of aggression, such as hate and stalking (29%).
Most of the respondents encountered new forms of aggression (hate and stalking) at work "rarely", i.e. 1-2 times a year (67.0%), but according to their observations, this form is becoming more and more frequent.
Almost ¾ of the respondents stated that aggression is a big problem for them (72.0%) and that it affects the bio-psycho-social well-being of healthcare workers, causing nervousness (26.0%) or discouragement and the need to change their attitude to work (18.0%). Detailed data are presented in Table V.
Tabel V.
| No. | The impact of aggression on bio-psycho-social well-being | % |
|---|---|---|
| 1. | nervousness | 26% |
| 2. | sleep disorders | 10% |
| 3. | drug abuse | 2% |
| 4. | nutrition problem | 4% |
| 5. | anxiety, depression | 9% |
| 6. | family relationship disorders | 5% |
| 7. | intimate life disorders | 1% |
| 8. | conflicts in the team | 9% |
| 9. | discouragement from work / change in attitude towards work | 18% |
| 10. | change of job | 5% |
| 11. | resignation from the profession | 4% |
| 12. | accidents at work (personal injuries) | 4% |
| 13. | professional exposures (infections) | 3,0% |
| Sum: | 100% |
Source: Own study.
In terms of knowledge and education, according to the conducted research, the vast majority of respondents had knowledge about the proper conduct with an aggressive patient, or after this phenomenon towards medical personnel (85.0%). However, the respondents declared the need for this type of training in each of the examined departments/unit of the workplace. The above issue is related to the knowledge of the use of direct coercion to ensure the patient, other patients and the staff of the medical facility safety and the appropriate quality of services (85.0%). The majority of respondents claimed that they were able to note the use of direct coercion towards aggressive patients (83%). Despite this, the majority declared that they liked their professional work (99.0%) and would not change it (83.0%). In stressful situations related to patient aggression they often had thoughts of quitting their professional work shortly after the incident (79.0%). The research hypotheses established in the work were confirmed by the results of the research.
Based on the results of the conducted research, the following conclusions were drawn:
1. Physical and verbal aggression from patients continued to be a very common phenomenon in healthcare.
2. Medical staff often experience particularly psychological aggression from patients and/or their relatives.
3. According to the respondents, new forms of aggression from patients and their families towards medical personnel were experienced, such as hate or stalking, but they occurred sporadically.
4. Aggression by patients towards medical staff always leaves negative health effects on them, mainly in the emotional sphere.
5. The surveyed medical personnel demanded continuous training on how to deal with aggressive patients.
In summary, the presented research results indicate that aggression in healthcare is a huge problem, and implementing new forms of stopping it is a necessary process enabling the proper functionality of healthcare workers. The research has shown that the problem is growing and should be constantly monitored and that staff should be constantly trained in their defense rights. It is advisable for employees of various medical professions to undertake mandatory education in the form of various classes, including workshops with psychological and pedagogical training. The education is intended to equip medical staff with new skills in dealing with aggressive patients and to strengthen proper interpersonal communication. Additionally, it will strengthen conflict resolution skills, providing broadly understood support.
1) Piotrowicz D., Aggression and violence as a social problem», ZSO No. 4, Gdynia 2019.
2)WHO, 2010, World Health Organization, World Health Statistics 2010.
3)Moczydłowska A, The phenomenon of professional burnout in the area of challenges of contemporary nursing, Monograph, MANS publishing house in Łomża; ŻPU named after Ivan Franko, 2024, pp.332-356.
4)Drabek M., Merecz D., Mościcka A., Scale of exposure to aggression at work among health care and service sector employees, Medycyna Pracy 2007, 58(4); pp. 299-306.
5)Bogucka M., Is it safe in Polish hospitals? Aggression and violence against staff, Evereth News 2020.
6)Steciwko A., Barański R., Mastalerz-Migas A., Aggression in health care, Issues Wrocław, 2014.
7)Frydrysiak K., Ejdukiewicz J., Grześkowiak M., Aggression of patients and their relatives towards the staff of the hospital emergency department, Anesthesiology and Rescue, 2016, 10, pp. 46-52.
8)https://oipip.lomza.pl/monitorowanie-agresji-w-ochronie-zdrowia/
9)https://nipip.pl/procedura-postepowania-pielegniarkipoloznej-objetej-ochrona-przewidziana-dla-funkcjonariusza-publicznego-przypadku-agresywnego-zachowania-pacjentarodziny/
10)https://nipip.pl/procedura-postepowania-pielegniarkipoloznej-objetej-ochrona-przewidziana-dla-funkcjonariusza-publicznego-przypadku-agresywnego-zachowania-pacjentarodziny/
11)Act of 15 July 2011 on the professions of a nurse and a midwife (Journal of Laws No. 174, item 1039, as amended).
12)Act of 6 June 1997 – Penal Code (Journal of Laws No. 88, item 553, as amended).
13)Śledziona M., Difficult patient, Nurse and Midwife Magazine no. 7-8, Warsaw 2021.
14)Bogucka M., Is it safe in Polish hospitals? Aggression and violence against staff, Evereth News 2020.
15)Lickiewicz J., Marzęcka A., Makara – Studzińska M., Comparative analysis of aggressive behavior in the emergency department and the surgery department – preliminary report, Anesthesiology and Rescue 2018, 12, pp. 266-273.
16)Hans S., Needham I., Abderhalben C., The effect of a training course on menthal health nurse attitudes on the reasons of patient aggression and its management, Journal of Psychiatric and Mental Health Nursing, 2006, 13(2), 197-220.
17)https://politykazdrowotna.com/artykul/w-czasie-pandemii-przybylo-agresji-w-szpitalachi przychodniach/824959.
18)Labor Code, Journal of Laws 2023.1465.
19)Zhu Y, Chen L, Ji H, et al. The Risk and Prevention of Novel Coronavirus Pneumonia Infections Among Inpatients in Psychiatric Hospitals. Neurosci Bull 2020; 36:299.
20)Ibidem.
21)Bilgin H., Tulek Z., Ozcan N., Psychometric properties of the Turkish version of the Perception of Agression Scale. J. Psychiatr Ment Health Nurs.
22)Kózka M., Lenartowicz H., Research methodology in nursing, Warsaw 2010, pp. 74–75, 97–98, 103–104.
Bogucka M. (2020). Is it safe in Polish hospitals? Aggression and violence against staff. Evereth News.
Drabek M., Merecz D., Mościcka A. (2007). Scale of exposure to aggression at work among health care and service sector employees. Medycyna Pracy, 58(4), 299-306.
Frydrysiak K., Ejdukiewicz J., Grześkowiak M. (2016). Aggression of patients and their relatives towards the staff of the hospital emergency department. Anesthesiology and Rescue,10.
Hans S., Needham I., Abderhalben C. (2006). The effect of a training course on menthal health nurse attitudes on the reasons of patient aggression and its management. Journal of Psychiatric and Mental Health Nursing, 13(2).
Polityka Zdrowotna. (2021, listopad 30). W czasie pandemii przybyło agresji w szpitalach i przychodniach. Polityka Zdrowotna. https://politykazdrowotna.com/artykul/w-czasie-pandemii-przybylo-agresji-w-szpitalach-i-przychodniach/824959
Okręgowa Izba Pielęgniarek i Położnych w Łomży. (n.d.). Monitorowanie agresji w ochronie zdrowia. OIPIP Łomża. https://oipip.lomza.pl/monitorowanie-agresji-w-ochronie-zdrowia/
Naczelna Izba Pielęgniarek i Położnych. (n.d.). Procedura postępowania pielęgniarki/położnej objętej ochroną przewidzianą dla funkcjonariusza publicznego w przypadku agresywnego zachowania pacjenta/rodziny. NIPIP. https://nipip.pl/procedura-postepowania-pielegniarkipoloznej-objetej-ochrona-przewidziana-dla-funkcjonariusza-publicznego-przypadku-agresywnego-zachowania-pacjentarodziny/
Ustawa z dnia 26 czerwca 1974 r. Kodeks pracy. (2023). Dziennik Ustaw, 2023, poz. 1465.
Lickiewicz J., Marzęcka A., Makara – Studzińska M. (2018). Comparative analysis of aggressive behavior in the emergency department and the surgery department – preliminary report. Anesthesiology and Rescue,12.
Moczydłowska, A. (2024). The phenomenon of professional burnout in the area of challenges of contemporary nursing. In Monograph (pp. 332–356). MANS Publishing House in Łomża; ŻPU named after Iwan Franko.
Steciwko, A., Barański, R., & Mastalerz-Migas, A. (2014). Aggression in health care: Introductory issues. Wrocław.
Spleen, M. (2021). Difficult patient. Nurse and Midwife Magazine, 7-8. Warsaw.
Ustawa z dnia 15 lipca 2011 r. o zawodach pielęgniarki i położnej. (2011). Dziennik Ustaw, Nr 174, poz. 1039, z późn. zm.
Ustawa z dnia 6 czerwca 1997 r. – Kodeks karny. (1997). Dziennik Ustaw, Nr 88, poz. 553, z późn. zm.
World Health Organization (WHO). (2010). World health statistics 2010. WHO.
Wojnicka, D., & Włoszczak-Szubzda, A. (2017). Knowledge and skills of medical staff in relation to manifestations of aggression on the part of the patient. Aspects of Health and Disease, 2(2).
Zhu, Y., Chen, L., Ji, H., et al. (2020). The risk and prevention of novel coronavirus pneumonia infections among inpatients in psychiatric hospitals. Neuroscience Bulletin, 36, 299. https://doi.org/10.1007/s12264-020-00406-9